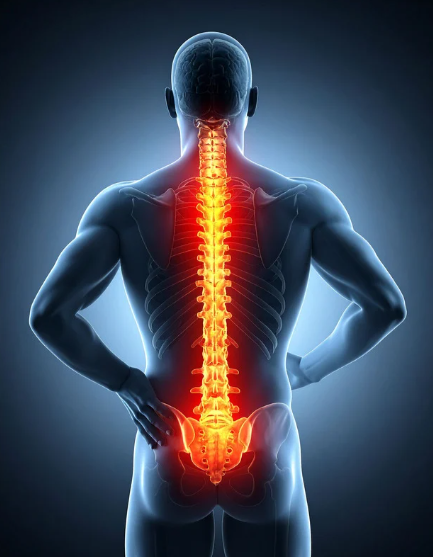
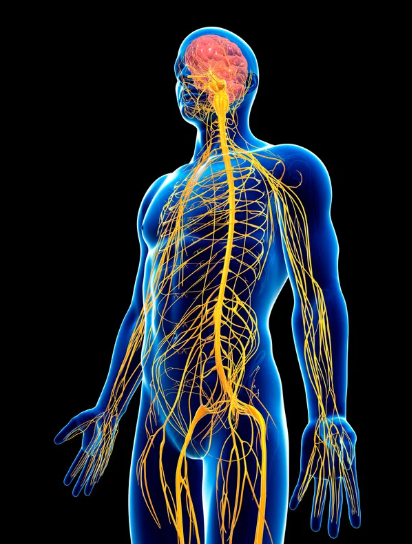
Men’s Pelvic Pain
Many men with pelvic pain suffer in silence, unsure where to turn or who can help. If this is you, please know that you are not alone. Pelvic pain in men is more common than many people realise, and help is available. This page brings together information, resources, and practical options to support you in understanding your pain and finding ways to manage it.
There is hope, and there are steps you can take toward feeling better.
Men and Pelvic Pain
Men with pelvic pain have a wide range of different symptoms for a variety of different reasons. Sometimes the pain starts after an injury, sometimes after a period of severe stress, or sometimes with no known cause.
Even knowing what to call the problem can be confusing, with a mix of different names often used, including Chronic Pelvic Pain Syndrome, Chronic Prostatitis, or Chronic Urogenital Pain Syndrome. Men with pelvic pain often suffer in silence, unsure of where to go, and unsure who can help them. You are not alone, there are many men with the same problem, and there are many things you can do to help with the pain.
The symptoms men describe vary widely, but may include:
Individuals may experience pain associated with sitting, walking, physical contact, or wearing tight clothing, which can involve the pelvis, penis, scrotum, perineum (the area between the scrotum and anus), pubic region, lower back, tailbone (coccyx), hips, groin, abdomen, bottom, rectum, or anus. This pain may be described as pressure, throbbing, aching, or burning in nature, including burning sensations affecting the penis, scrotum, or crotch.
Structural pain may arise from involvement of the hips, groin, lower back, tailbone (coccyx), or abdominal region and is often related to musculoskeletal or joint-based contributors that may affect posture, movement, or load tolerance.
Functional pain commonly presents as pelvic pain or pressure, throbbing or aching sensations within the pelvis or genital region, and burning pain involving the penis, scrotum, crotch, or perineum. Symptoms may be exacerbated by prolonged sitting, light touch, or clothing contact and are frequently associated with pelvic floor dysfunction, nerve sensitivity, or altered pain processing.
Bowel-related symptoms may include pain during bowel movements, a persistent sensation of incomplete emptying, difficulty or inability to pass wind, anal or rectal pain, bloating, altered bowel habits such as diarrhoea and/or constipation, and food intolerances that may worsen symptoms.
Bladder symptoms may include features consistent with painful bladder syndrome, such as bladder or pelvic pain, discomfort during urination, a slow or interrupted urinary stream, and increased urinary frequency or urgency.
Sexual symptoms may include pain during intercourse, erections, ejaculation, or orgasm, as well as reduced libido and erectile difficulties, which can significantly affect sexual function and quality of life.
The ongoing presence of symptoms may contribute to social withdrawal, reduced self-esteem, low energy levels, behavioural or emotional changes, and the development or exacerbation of anxiety and depressive symptoms.
Whereas pelvic pain often starts in the teenage years for women, it generally starts at an older age in men, and may have been present for a shorter time.
A series of 112 men with pelvic pain assessed in a pelvic physiotherapy clinic in Melbourne showed that:
the age of those affected varied from 19-84 years with an average age of 41 years
pain had been present for less than 12 months in 57%, 12-24 months in 21% and over 2 years in 22%
80% of men described their stress levels as high, 20% as normal
pain was described as Testicular in 66%, Perineal in 65%, Penile in 46%, Suprapubic in 36%, Rectal in 29%, Hip/groin in 25%, Lumbar spine in 14%, and Buttocks in 9%.
(1) Morrison S, Erm J, Brownhill J. Audit of Mens Pelvic Pain 2009–2012. Womens and Mens Physiotherapy, Malvern
(2) Jason A. Ferris, Marian K. Pitts, Juliet Richters, Judy M. Simpson, Julia M. Shelley and Anthony M. Smith. National prevalence of urogenital pain and prostatitis-like symptoms in Australian men using the National Institutes of Health Chronic Prostatitis Symptoms Index. BJU Int 2009 105; pp.373-379
Chronic Prostatitis
The prostate is a small gland, around the size of a walnut, that’s only found in men. It lies just underneath the bladder and surrounds the top part of the urethra. It makes fluid that protects and feeds sperm, which is around 1/3 of the fluid ejaculated at orgasm. If the prostate gland becomes inflamed, this is called Prostatitis.
A short-term infection is called Acute Prostatitis. This usually gets better after a few days, or possibly weeks, of antibiotics.
A longer-term infection is called Chronic Prostatitis. This is much less common – maybe 10% of prostatitis cases.
Over the years, pelvic pain in men has consistently been blamed on Chronic Prostatitis. While Prostatitis can cause pelvic pain and may have been present at some stage, we now know that Chronic Prostatitis is present in only a small number of men with long-term pelvic pain.
How is Prostatitis diagnosed?
Men with prostatitis due to infection will have bacteria found in their urine or prostatic secretions – so tests for infection should be positive. If these tests are negative, and he was not using antibiotics at the time of testing, then prostatitis is much less likely. It is important to check for prostatitis but to recognise that there are other causes of pelvic pain in men too.
If it isn’t Prostatitis, what else could be causing the pain?
For reasons that are not well understood, some men start with pain in one organ and then develop pain from overly tight pelvic muscles and sensitised nerves. This results in the situation now called Chronic Pelvic Pain Syndrome (CPPS). This condition is poorly understood and often not recognised because it doesn’t show on scans or at an operation. Unfortunately, many men are treated with antibiotics for ‘Chronic Prostatitis’ for a long time when no infection is present.
There are many conditions that can initiate CPPS and many different symptoms. Typically, the pain is present on most days for at least 3 months. Affected men might complain of any of the following symptoms:
Pelvic pain – in the perineum, testicles, the tip of the penis, abdomen (pubic / bladder area)
– Constant burning pain in the penis
– Tenderness – pain on touch, sitting, walking or wearing tight underwear
– Arthralgia/ myalgia (joint/ muscle pain including back pain)Bladder troubles
– Dysuria (painful urination)
– Frequency or urgency of passing urine (possible Painful Bladder Syndrome)Bowel troubles
– Irritable Bowel Syndrome (constipation, diarrhoea, bowel pain)
– Food intolerancesSexual difficulties
– Low libido (reduced sex drive)
– Post-ejaculatory pain (pain after ejaculating)
– Pain on erection or erectile difficulties
Are my pain troubles the same ones that many older men complain of?
Generally, no. As men age, the prostate enlarges. This narrows the urethra making it harder to pass urine. They feel the need to pass urine more frequently, and the urine stream is slower. It does not mean that the prostate is inflamed (prostatitis) or that they have CPPS. Men with pelvic pain may have a slow urine stream too, but this is generally because the pelvic floor muscles are tight or in spasm. When the pelvic muscles learn to relax, the urine stream improves.
“I had pelvic pain for four years! My private regions were so sensitive to touch that when the doctor examined my rectum it was like murder! At first, I started having urinary frequency where I had to go to the toilet every 30 minutes. Then it started hurting every time I passed bowel motions. It was difficult to have sex because I had pain when I had an erection or ejaculated. Even sitting down or walking with hard shoes was unbearable and I had to wear loose-fitting underwear. After seeing multiple doctors and urologists and having a dozen investigations come back normal, everyone said there was nothing wrong with me.””
What is Chronic Pelvic Pain?
A pain may start in a pelvic organ such as your bladder, bowel, or prostate following an infection, or in your pelvic muscles following an injury. It is important to see your doctor to exclude serious diseases and to appropriately treat these conditions that may lead to pain. Sometimes no cause is found and pelvic pain may start during a period of severe stress. Whatever the original cause of pain, if it does not settle then the pain can become chronic even when the original infection or injury has resolved. Generally, pelvic pain is considered ‘chronic’ if it is present for most days for at least 3-6 months. No-one completely understands why a similar condition in some men might lead to chronic pain, while in another man it might go away completely.
Once a pain has become chronic, the pain situation is usually more complicated. For unknown reasons, the body continues to believe the issue is still present, even when the initial injury or infection has resolved, and interprets this as pain. Surrounding pelvic muscles can tighten in attempt to protect the body from further damage as a defence mechanism. When these muscles are constantly tensed, shortened and tight, they start aching and can spasm. Often the pain from pelvic muscle spasms can become the worst part of the pain.
Additionally, nerve pathways that send pain messages through the spinal cord to the brain can become sensitised due to constant signalling and experience of pain. In some cases, even a brush of a feather can be interpreted as unbearable pain, this is referred as hyperalgesia.
Once muscles and nerves in the pelvis start behaving abnormally, other organs can develop problems too. Pelvic floor muscles control bladder and bowel motions by tightening to stop urine or stool passing and relaxing to allow us to urinate or defecate (open your bowels) when appropriate. Trying to urinate, defecate, or ejaculate through painful tight pelvic muscles that cannot relax normally can be extremely painful.
Stress, anxiety and depression can also sensitise pain nerve pathways, particularly in the brain, further enhancing the experience of pain. For example, stubbing your toe will hurt more on a bad day than on a good day. Unfortunately, it is not uncommon for people to become depressed from the effects of pain has on their functionality, productivity, sleep, relationships and quality of life, which can further worsen the pain. This can become a vicious cycle as pain can dampen your mood and depression worsens the experience of pain with further impairment on productivity and quality of life.
How does Chronic Pelvic Pain Syndrome develop?
There’s a lot still to learn about CPPS. In some men, stressors or anxiety result in excessive pelvic muscle tension (causing pain) and excessive pain signalling via the pelvic nerves (increased pain sensitivity).
Pelvic Floor muscles work best when they can tighten and relax normally. They control bladder and bowel motions by tightening to stop urine or stool passing and then relaxing to allow us to urinate or defecate (open your bowels) when appropriate. When these muscles are constantly tensed, shortened and tight, they start hurting and can go into spasm. Trying to pass urine or a bowel action past painful tight pelvic muscles that can’t relax normally is extremely painful.
Anyone who has had pain of some kind on most days for more than 3-6 months will develop changes in the spinal cord that result in pain sensitivity. With these changes come other symptoms such as anxiety, low mood, nausea, dizziness, fatigue and poor sleep.
How can I manage Chronic Pelvic Pain?
There are many self-help techniques you can use to manage your pain. The suggestions below are all techniques used successfully by men to manage pelvic pain.
1. Manage the original cause of your pain if this can be determined - This is usually a problem with one of the pelvic organs, although there is sometimes no obvious cause. See your doctor to exclude serious diseases.
2. Learn more about your pain - If your pain has been fully assessed by your doctor and no serious disease has been found; you may understand that you aren’t in danger but still do not how to manage your pain. Everyone is different, it is important to learn more about your individual condition – why you have pain, where it is coming from, and what are the things that make your pain better or worse. Increased understanding of the condition and pain can help reduce the fear, stress and anxiety surrounding your pain. This empowers you to take control of your pain, rather than allowing your pain to control your life.
Maybe your pain is brought on by sitting or standing for more than thirty minutes, wearing tight jeans or when you had a stressful day. Maybe your pain improves when you stretch and have a nice relaxing bath after a long day at work. It is a good idea to make a list of your problems and record the activities that improve or worsen your pain, and which treatments helped you most.
3. Pace your activities - Sometimes ongoing pain can cause us to alter activity levels, which can be helpful short term but not long term. Fear of pain flares can mean we avoid things, including the things that can help with our pain.
Others do too much when they feel good (boom) and then cannot do much for a while (bust) due to the pain flare from the overexertion. Doing too much or too little can lead to more pain and less function. Finding the middle road by pacing can be helpful.
Activity pacing involves breaking activities into smaller manageable chunks with regular breaks gradually increasing intensity. This allows you to conserve more energy to get more done with overall less discomfort. Pacing empowers you to have more control of your life, allowing you to do the things that are important to you.
Try to do activities up to 80% effort, with a gradual increase of 10 % increase in action each week with regular rest breaks in between. For example, if you know pain or fatigue sets in after 10 minutes of walking, limit your walking to 8 minutes with regular breaks. Increase the duration of walking by 1 minute each week. This allows you to walk every day, rather than walking for one day and recovering for multiple days.
If you flare, try not to panic! Sensitive nervous systems may flare to protect you, but it does not necessarily mean you are injured. Go back to a level you can manage and start pacing up again. Remember to take one step at a time; consistency is more important than intensity.
Click the Live Well with Pain image to download a guide and an Activity Diary.
4. Learn where your pelvic muscles are and learn to move them normally - No matter how the pain started, if you have pain on most days, it is likely that your pelvic floor muscles are constantly tensed without you realising. When muscles stay tight, they get painful and can spasm. Reducing the tension in the muscles of your pelvic floor through relaxing and stretching exercises allows the muscles to work normally again, reducing your pain and potentially improving bladder, bowel, and sexual function. It is also important to have good bowel and bladder habits to take pressure off your pelvic muscles. Bowels should work efficiently without straining, and emptying should not be painful.
The pelvic floor muscles lie across the bottom of your pelvis like a trampoline. On top of the muscular trampoline lies the bladder and rectum. The pelvic floor muscles need to relax to be able to pass urine, bowels or semen. The trampoline sags and moves down when it relaxes and tightens and moves up as it contracts.
You can learn to move your pelvic muscles normally by the following steps:
Stand in front of the mirror without your underwear
Lift your testicles gently towards your body by tightening your pelvic muscles. You may notice your penis retract as you tighten ( be careful as this can worsen your pain, so do it gently or skip this movement altogether).
Now relax your pelvic floor and let the testicles hang loose again. Concentrate on loosening and softening the muscles in and around your pelvis. Taking a big breath in and letting your belly hang loose may help relax your pelvis.
Think about how your anus tightens and loosens with the above movements. Up movement of the pelvic floor causes it to close, and down movement causes it to loosen.
The relaxing and loosening part of this exercise is most important for you. It may not be easy at first, but regular practice and training will make it easier. Excessive tightening may worsen pain, so be gentle when you first start this.
5. Learn to relax the pelvic floor muscles and your mind using special stretches and whole body guided relaxation - Targeted stretches will help reduce tension and pain in and around the pelvis. If you need help, you can seek help from a pelvic floor physiotherapist. Click the image for a download of pelvic stretches you can do.
Whole body relaxation is good for identifying muscles you habitually and subconsciously hold tight and tense. Guided relaxation exercises and stretches help reduce the tension in other muscles as well as your pelvic floor muscles and are good for managing your stress.
6. Calm your nervous system, to reduce the pain sensitisation - Stress, anxiety and depression can worsen your pain. Learn to manage your stress to improve your pain. Using the same techniques for pain, try to identify the things that worsen and improve your stress. Additionally, getting good sleep, regular appropriate physical activity, and a healthy diet will help with stress. There are several online self-paced courses you can access to help manage stress, anxiety and pain. Visit https://thiswayup.org.au/ for some courses. This Way Up Chronic Pain course requires a referral from your GP to make the program free. The
Medications such as amitriptyline, duloxetine, and pregabalin/ gabapentin can help calm your nervous system and reduce pain sensitisation and hyperalgesia. It is important to avoid opiate medications such as oxycodone and panadeine forte. Although they help in the short term, opioids can worsen the pain in the long term and have many associated issues, including dependence, tolerance, and addiction. See your doctor for further advice.
A word of advice about other exercise
It’s good to keep fit but some of the exercises you do could be making your pain worse. Exercises such as core strengthening, heavy weights from a deep squat, high impact exercise or cycling can all make the pelvic floor muscles tighter – and more painful. It may be helpful to stop these types of exercises for a while. Instead, you could use a cross trainer, walk on a treadmill, swim and add stretches to your program. This site has a page of yoga stretches for men, which can help. A pelvic floor physiotherapist, experienced in pelvic pain can advise you on exercise suited to your needs.
Karl Monahan is a sports and advanced clinical massage therapist. He has extensive training in abdominal and pelvic health and has successfully treated males with chronic prostatitis and chronic pelvic pain syndrome since 2009.
Karl shares his personal experience with chronic testicular and pelvic pain.
Karl recommends all his patients to identify DIMs and SIMs “Danger (signals) In Me” and “Safety (signals) in Me”. Read more here.
For more in-depth information about the diagnosis and treatment of male pelvic pain, watch Ms Shan Morrison’s presentation at the Pelvic Pain Foundation of Australia Health Practitioner Training Seminar 2018.
Ms Shan Morrison is a Pelvic Floor Physiotherapist in Melbourne who is highly experienced in the management of pelvic pain.
Read more of Shan Morrison’s research contributions here.

Pelvic Pain Conditions affecting Men
-
Bands of internal scar tissue (often after surgery or inflammation) that can tug on tissues and contribute to ongoing abdominal or pelvic discomfort.
-
Overstretched or torn abdominal muscles (often from lifting, sport, or sudden movement) that can cause lower abdominal or pelvic pain, usually worse with activity.
-
A small tear in the anal lining that becomes slow-healing, causing ongoing pain (often with bowel movements) and pelvic floor tension.
-
A bulge in a major blood vessel in the abdomen or pelvis. It can occasionally cause deep pelvic or back pain. This is uncommon, but it’s an important condition doctors may consider when symptoms fit.
-
Sometimes called a sports hernia. A strain or tear of soft tissues in the lower abdomen or groin (without a true hernia in many cases). Common in athletes and can cause persistent groin/pubic/pelvic pain.
-
A non-cancerous enlargement of the prostate that can affect urine flow and create a sense of pelvic pressure or discomfort.
-
Can sometimes cause persistent pelvic discomfort, often with urinary changes such as blood in the urine.
-
Pelvic or perineal pain lasting 3 months or more, often with urinary and/or sexual symptoms, where no ongoing infection is identified.
-
Repeated or long‑lasting bacterial infection of the prostate gland that can cause pelvic pain and urinary symptoms, often with fever or feeling unwell, over months.
-
Persistent prostate-area symptoms (pelvic pain, urinary and/or sexual symptoms) where no ongoing bacterial infection is found; often overlaps with CPPS.
-
Testicular or scrotal pain lasting 3 months or more; may be local, nerve-related, or referred from the pelvis, hip, or spine.
-
A hernia that becomes trapped (and in strangulation, has compromised blood supply). This is uncommon but important, and typically causes significant pain and a tender lump.
-
A bulge through the lower abdominal wall into the groin that can cause ongoing aching or pressure in the groin/pelvis, often worse with lifting or coughing.
-
Ongoing bladder-area pain or pressure with urinary urgency/ frequency, without an active infection.
-
A common long-term gut–brain condition causing cramping, bloating, and bowel habit changes; pelvic discomfort can be part of the pattern.
-
Pelvic floor muscle spasm/tension causing deep rectal or pelvic aching, often worse with sitting.
-
Narrowing around spinal nerves that can cause ongoing back pain with referred pelvic/groin discomfort.
-
Irritation of nerves in the lower spine that can refer persistent pain into the groin or pelvis, sometimes with back or leg symptoms.
-
Irritation of the obturator nerve causing persistent deep groin pain and inner-thigh pain, sometimes felt as pelvic pain.
-
Inflammation and irritation around the pubic joint (front of the pelvis), often from overuse; can cause persistent pubic and pelvic pain.
-
Tumours in pelvic bones can cause deep, persistent pelvic pain; uncommon, but sometimes considered in evaluations of long-lasting pain.
-
Overactive or tense pelvic floor muscles causing persistent pelvic/perineal pain and sometimes urinary, bowel, or sexual symptoms.
-
Pain that persists for months after surgery (such as hernia repair), sometimes due to nerve irritation, scar tissue, or ongoing muscle guarding.
-
Ongoing testicular/scrotal/groin pain for 3 months or more after vasectomy; may relate to congestion, inflammation, or nerve sensitivity.
-
Inflammation of the anal rectal lining that can cause rectal pain, bleeding, diarrhoea, feeling as if there is a need to have a bowel movement, and discomfort that may be felt as pelvic pain.
-
Can sometimes cause persistent pelvic discomfort, particularly in more advanced disease; many people have other symptoms, or none early on. Often pain is minimal.
-
Irritation of the pudendal nerve causing persistent burning, aching, or sharp pain in the perineum/genitals, often worse with sitting.
-
A growth behind the abdominal lining that can cause persistent referred pelvic or groin pain; uncommon.
-
Pain from the joint between the spine and pelvis that can persist and refer into the buttock, groin, or pelvic area.
-
A cyst in the epididymis. Often painless, but can cause a long-term heavy or aching sensation in the scrotum/groin.
-
A condition affecting spinal nerves that can cause persistent referred pelvic pain and neurological symptoms; uncommon.
-
Twisting of the spermatic cord causing sudden severe pain; needs urgent medical assessment.
-
A stone moving down the ureter can cause intense pain that often radiates to the groin and may be felt as pelvic pain.
-
Scarring that narrows the urethra and can cause ongoing urinary symptoms and pelvic/perineal discomfort.
-
Enlarged veins around the testicle that can cause a long-term dull ache or heaviness, often worse after standing or exercise.
-
Can cause persistent pelvic or lower abdominal discomfort in some cases, often with bowel changes or bleeding.
-
Inflammation or infection of small pouches in the bowel wall, often causing lower abdominal/pelvic pain and sometimes fever or bowel changes.
-
Inflammation or infection of the epididymis (the tube behind the testicle). Pain may be felt in the scrotum and can radiate into the groin or pelvis.
-
Inflammation or infection involving both the epididymis and the testicle, often causing scrotal pain and swelling that may refer into the pelvis.
-
A hernia in the upper thigh/groin region that can cause ongoing groin or pelvic discomfort, especially with standing or straining.
-
A hip-joint shape mismatch that can pinch with movement, often causing long-term groin or pelvic pain and stiffness.
-
Irritation of a nerve supplying the groin and genitals, causing persistent burning, aching, or sharp pain in the lower abdomen/groin/scrotum.
-
Swollen veins around the anus that can cause ongoing pain, pressure, or discomfort (sometimes described as rectal or pelvic pain).
-
A rare pattern of symptoms where the penis may feel firmer while flaccid, often with pelvic/perineal pain and changes in erections, sensation, or urination.
-
Wear-and-tear change in the hip joint that can cause persistent groin or pelvic pain, stiffness, and reduced range of motion.
-
Fluid around a testicle. Many are painless, but some cause a long-term heavy or aching feeling that may radiate into the groin.
-
Crohn’s disease or ulcerative colitis. Long-term inflammatory conditions that can cause recurrent or persistent abdominal/pelvic pain with bowel symptoms.